Bongwarrior (talk | contribs) m Reverted edits by 213.84.202.89 (talk) to last version by 137.144.145.25 |
123.200.168.108 (talk) it's not about TCM, tightened language, removed spin |
||
| Line 19: | Line 19: | ||
'''Acupuncture '''(from Lat. ''acus,'' "needle", and ''pungere,'' "to prick") or in [[Standard Mandarin]], 針砭 (zhēn biān) (a related word, 針灸 (zhēn jiǔ), refers to acupuncture together with [[moxibustion]])<ref>ABC Chinese-English Comprehensive Dictionary edited by John DeFrancis, as used in [http://www.wenlin.com/ Wenlin] version 3.4.1</ref> is a technique of inserting and manipulating fine [[wikt:filiform|filiform]] needles into specific points on the body with the aim of relieving [[pain]] and for therapeutic purposes.<ref name="Dorlands">'''Acupuncture''': the Chinese practice of piercing specific areas of the body along peripheral nerves with fine needles to relieve pain, induce surgical anesthesia, and for therapeutic purposes. ''Dorland's Pocket Medical Dictionary'', 25th ed. W. B. Saunders Co., 1995. ISBN 0-7216-5738-9</ref> According to [[traditional chinese medicine|traditional Chinese medical theory]], these [[acupuncture points]] lie along [[Meridian (Chinese medicine)|meridians]] along which [[qi]], the [[vital energy]], flows. There is no known [[anatomical]] or [[histological]] basis for the existence of [[acupuncture points]] or meridians.<ref name="Mann F.">[[Felix Mann]]. ''[http://www.chinesemedicinetimes.com/section.php?xSec=122 Chinese Medicine Times]'', vol 1 issue 4, Aug. 2006, "The Final Days of Traditional Beliefs? - Part One"</ref><ref name="NIH-1997consensus"/> Modern acupuncture texts present them as ideas that are useful in clinical practice.<ref name="Bensky Shanghai p.35" /><ref>Cheng Xinnong. Chinese Acupuncture and Moxibustion, p. 53. Foreign Languages Press, 1987 (First edition; Fourth Printing, 1996). ISBN 7-119-00378-X</ref><ref>Kaptchuk, ''The Web That Has No Weaver'', 1983, pp. 34-35</ref> According to the [[NIH]] consensus statement on acupuncture, these traditional Chinese medical concepts "are difficult to reconcile with contemporary biomedical information but continue to play an important role in the evaluation of patients and the formulation of treatment in acupuncture."<ref name="NIH-1997consensus"/> |
'''Acupuncture '''(from Lat. ''acus,'' "needle", and ''pungere,'' "to prick") or in [[Standard Mandarin]], 針砭 (zhēn biān) (a related word, 針灸 (zhēn jiǔ), refers to acupuncture together with [[moxibustion]])<ref>ABC Chinese-English Comprehensive Dictionary edited by John DeFrancis, as used in [http://www.wenlin.com/ Wenlin] version 3.4.1</ref> is a technique of inserting and manipulating fine [[wikt:filiform|filiform]] needles into specific points on the body with the aim of relieving [[pain]] and for therapeutic purposes.<ref name="Dorlands">'''Acupuncture''': the Chinese practice of piercing specific areas of the body along peripheral nerves with fine needles to relieve pain, induce surgical anesthesia, and for therapeutic purposes. ''Dorland's Pocket Medical Dictionary'', 25th ed. W. B. Saunders Co., 1995. ISBN 0-7216-5738-9</ref> According to [[traditional chinese medicine|traditional Chinese medical theory]], these [[acupuncture points]] lie along [[Meridian (Chinese medicine)|meridians]] along which [[qi]], the [[vital energy]], flows. There is no known [[anatomical]] or [[histological]] basis for the existence of [[acupuncture points]] or meridians.<ref name="Mann F.">[[Felix Mann]]. ''[http://www.chinesemedicinetimes.com/section.php?xSec=122 Chinese Medicine Times]'', vol 1 issue 4, Aug. 2006, "The Final Days of Traditional Beliefs? - Part One"</ref><ref name="NIH-1997consensus"/> Modern acupuncture texts present them as ideas that are useful in clinical practice.<ref name="Bensky Shanghai p.35" /><ref>Cheng Xinnong. Chinese Acupuncture and Moxibustion, p. 53. Foreign Languages Press, 1987 (First edition; Fourth Printing, 1996). ISBN 7-119-00378-X</ref><ref>Kaptchuk, ''The Web That Has No Weaver'', 1983, pp. 34-35</ref> According to the [[NIH]] consensus statement on acupuncture, these traditional Chinese medical concepts "are difficult to reconcile with contemporary biomedical information but continue to play an important role in the evaluation of patients and the formulation of treatment in acupuncture."<ref name="NIH-1997consensus"/> |
||
Acupuncture originated in [[China]] and is most commonly associated with [[traditional Chinese medicine]] (TCM) |
Acupuncture originated in [[China]] and is most commonly associated with [[traditional Chinese medicine]] (TCM). Different types of acupuncture (Classical Chinese, Japanese, Tibetan, Vietnamese and Korean acupuncture) are practiced and taught in various parts of the world. |
||
While acupuncture has been |
While acupuncture has been studies scientifically since the late 20th century it remains controversial.<ref name="Ernst_2006-02"> {{cite journal |title=Acupuncture - a critical analysis |journal=Journal of Internal Medicine |date=2006-02 |first=Edzard |last=Ernst |volume=259 |issue=2 |pages=125–137 |pmid=16420542 |url=http://www.ncbi.nlm.nih.gov/pubmed/16420542?dopt=Abstract |accessdate=2008-04-08 |doi=10.1111/j.1365–2796.2005.01584.x }}</ref> The body of evidence remains inconclusive and a 2007 review by [[Edzard Ernst]] and colleagues finds that the "emerging clinical evidence seems to imply that acupuncture is effective for some but not all conditions."<ref name ="pmid17265547" /> |
||
The [[WHO]], the [[National Center for Complementary and Alternative Medicine]] (NCCAM) of the [[National Institutes of Health]] (NIH), the [[American Medical Association]] (AMA) and various government reports have all studied and commented on the efficacy (or lack thereof) of acupuncture. There is general agreement that acupuncture is safe when administered by well-trained practitioners using sterile needles, and that further research is appropriate.<ref name="NIH-1997consensus">{{cite web |author=NIH Consensus Development Program |title=Acupuncture --Consensus Development Conference Statement |url=http://consensus.nih.gov/1997/1997Acupuncture107html.htm |date=November 3-5, 1997 |publisher=National Institutes of Health |accessdate=2007-07-17}}</ref><ref name="NCCAM2006-Acupuncture">{{cite web |title=Get the Facts, Acupuncture |url=http://nccam.nih.gov/health/acupuncture/ |publisher=National Institute of Health |year=2006 |accessdate=2006-03-02}}</ref><ref name="pmid12801494">{{cite journal |author=Ernst G, Strzyz H, Hagmeister H |title=Incidence of adverse effects during acupuncture therapy-a multicentre survey |journal=Complementary therapies in medicine |volume=11 |issue=2 |pages=93–7 |year=2003 |pmid=12801494 |doi=}}</ref> |
The [[WHO]], the [[National Center for Complementary and Alternative Medicine]] (NCCAM) of the [[National Institutes of Health]] (NIH), the [[American Medical Association]] (AMA) and various government reports have all studied and commented on the efficacy (or lack thereof) of acupuncture. There is general agreement that acupuncture is safe when administered by well-trained practitioners using sterile needles, and that further research is appropriate.<ref name="NIH-1997consensus">{{cite web |author=NIH Consensus Development Program |title=Acupuncture --Consensus Development Conference Statement |url=http://consensus.nih.gov/1997/1997Acupuncture107html.htm |date=November 3-5, 1997 |publisher=National Institutes of Health |accessdate=2007-07-17}}</ref><ref name="NCCAM2006-Acupuncture">{{cite web |title=Get the Facts, Acupuncture |url=http://nccam.nih.gov/health/acupuncture/ |publisher=National Institute of Health |year=2006 |accessdate=2006-03-02}}</ref><ref name="pmid12801494">{{cite journal |author=Ernst G, Strzyz H, Hagmeister H |title=Incidence of adverse effects during acupuncture therapy-a multicentre survey |journal=Complementary therapies in medicine |volume=11 |issue=2 |pages=93–7 |year=2003 |pmid=12801494 |doi=}}</ref> |
||
Revision as of 14:41, 4 December 2008
| Acupuncture | |
|---|---|
| Medicine: | CAM |
| NCCAM: | Alternative Medical Systems[1] |
| NCCAM: | Energy Medicine[2] |
| Modality: | Professionalized |
| Culture: | East/West |

Acupuncture (from Lat. acus, "needle", and pungere, "to prick") or in Standard Mandarin, 針砭 (zhēn biān) (a related word, 針灸 (zhēn jiǔ), refers to acupuncture together with moxibustion)[3] is a technique of inserting and manipulating fine filiform needles into specific points on the body with the aim of relieving pain and for therapeutic purposes.[4] According to traditional Chinese medical theory, these acupuncture points lie along meridians along which qi, the vital energy, flows. There is no known anatomical or histological basis for the existence of acupuncture points or meridians.[5][6] Modern acupuncture texts present them as ideas that are useful in clinical practice.[7][8][9] According to the NIH consensus statement on acupuncture, these traditional Chinese medical concepts "are difficult to reconcile with contemporary biomedical information but continue to play an important role in the evaluation of patients and the formulation of treatment in acupuncture."[6]
Acupuncture originated in China and is most commonly associated with traditional Chinese medicine (TCM). Different types of acupuncture (Classical Chinese, Japanese, Tibetan, Vietnamese and Korean acupuncture) are practiced and taught in various parts of the world.
While acupuncture has been studies scientifically since the late 20th century it remains controversial.[10] The body of evidence remains inconclusive and a 2007 review by Edzard Ernst and colleagues finds that the "emerging clinical evidence seems to imply that acupuncture is effective for some but not all conditions."[11]
The WHO, the National Center for Complementary and Alternative Medicine (NCCAM) of the National Institutes of Health (NIH), the American Medical Association (AMA) and various government reports have all studied and commented on the efficacy (or lack thereof) of acupuncture. There is general agreement that acupuncture is safe when administered by well-trained practitioners using sterile needles, and that further research is appropriate.[6][12][13]
History
Antiquity
In China, the practice of acupuncture can perhaps be traced as far back as the Stone Age, with the Bian shi, or sharpened stones. Stone acupuncture needles dating back to 3000 B.C. have been found by archeologists in Inner Mongolia. [14][15] Clearer evidence exists from the 1st millennium BCE, and archeological evidence has been identified with the period of the Han dynasty (202 BC–220 AD).
Recent examinations of Ötzi, a 5,000-year-old mummy found in the Alps, have identified over 50 tattoos on his body, some of which are located on acupuncture points that would today be used to treat ailments Ötzi suffered from. Some scientists believe that this is evidence that practices similar to acupuncture were practiced elsewhere in Eurasia during the early Bronze Age. According to an article published in The Lancet by Dorfer et al., "We hypothesised that there might have been a medical system similar to acupuncture (Chinese Zhenjiu: needling and burning) that was practiced in Central Europe 5,200 years ago... A treatment modality similar to acupuncture thus appears to have been in use long before its previously known period of use in the medical tradition of ancient China. This raises the possibility of acupuncture having originated in the Eurasian continent at least 2000 years earlier than previously recognised."[16], [17].
Acupuncture's origins in China are uncertain. The earliest Chinese medical text that first describes acupuncture is the Yellow Emperor’s Classic of Internal Medicine (History of Acupuncture) Huangdi Neijing, which was compiled around 305–204 B.C. However, the Chinese medical texts (Ma-wang-tui graves, 68 BC) do not mention acupuncture. Some hieroglyphics have been found dating back to 1000 B.C. that may indicate an early use of acupuncture. Bian stones, sharp pointed rocks used to treat diseases in ancient times, have also been discovered in ruins; some scholars believe that the bloodletting for which these stones were likely used presages certain acupuncture techniques.[18]
According to one legend,[19], acupuncture started in China when some soldiers who were wounded by arrows in battle experienced a relief of pain in other parts of the body, and consequently people started experimenting with arrows (and later needles) as therapy.
Middle history
Acupuncture spread from China to Japan, Korea, Vietnam and elsewhere in East Asia. Portuguese missionaries in the 16th century were among the first to bring reports of acupuncture to the West.[20]
Modern era
Following the Revolution of 1911 in China, Western Medicine was introduced and acupuncture and Chinese herbology were in drastic decline. Due to the large population and need for medical care, acupuncture and herbs remained popular among the folk people, and later on with the emergence of "barefoot doctors."[21]
Acupuncture was used exclusively during the Long March and despite harsh conditions it helped maintain the health of the People's Liberation Army.[21] This led Mao Zedong, the leader of the Chinese Communist Party, to see that acupuncture remained an important element in China's medical system.[21] R.C. Crozier in the book Traditional medicine in modern China (Harvard University Press, Cambridge, 1968) says the early Chinese Communist Party leaders expressed considerable antipathy towards traditional Chinese medicine, ridiculing it as superstitious, irrational and backward, and claiming that it conflicted with the Party’s dedication to science as the way of progress. Acupuncture was included in this criticism. Reversing this position, Communist Party Chairman Mao Zedong later said that "Chinese medicine and pharmacology are a great treasure house and efforts should be made to explore them and raise them to a higher level."[22] In the late 1950s to the 1960s, acupuncture research continued with further study of the ancient texts, clinical effect on various diseases, acupuncture anesthesia, and acupuncture's effect on the internal organs.[21]
Representatives were sent out across China to collect information about the theories and practices of Chinese medicine. Traditional Chinese medicine is the formalized system of Chinese medicine that was created out of this effort. TCM combines the use of acupuncture, Chinese herbal medicine, tui na, and other modalities. After the Cultural Revolution, TCM instruction was incorporated into university medical curricula under the "Three Roads" policy, wherein TCM, biomedicine, and a synthesis of the two would all be encouraged and permitted to develop.
In Vietnam, Dr. Van Nghi and colleagues used the classical Chinese medical texts and applied them in clinical conditions without reference to political screening. They rewrote the modern version: Trung E Hoc.[clarification needed] Van Nghi was made the first President of the First World Congress of Chinese Medicine at Beijing in 1988 in recognition of his work.
From the 1970s to the present, acupuncture continues to play an important role in China's medical system,[21] and China has taken the lead in researching all aspects of acupuncture's application and clinical effects.[21]
In the 1970s, acupuncture became popular in America after American visitors to China brought back firsthand reports of patients undergoing major surgery using acupuncture as their sole form of anesthesia. The National Acupuncture Association (NAA), the first national association of acupuncture in the US, introduced acupuncture to the West through seminars and research presentations. The NAA created and staffed the UCLA Acupuncture Pain clinic in 1972. This was the first legal clinic in a medical school setting in the US.[citation needed] The first acupuncture clinic in the United States is claimed to have been opened by Dr. Yao Wu Lee in Washington, D.C. on July 9th, 1972.[23]
Traditional theory
Traditional Chinese medicine
Chinese medicine is based on a pre-scientific paradigm of medicine that developed over several thousand years. Its theory holds the following explanation of acupuncture:
Health is a condition of balance of yin and yang within the body. Particularly important in acupuncture is the free flow of Qi, a difficult-to-translate concept that pervades Chinese philosophy and is commonly translated as "vital energy". Qi is immaterial and hence yang; its yin, material counterpart is Blood (capitalized to distinguish it from physiological blood, and very roughly equivalent to it). Acupuncture treatment regulates the flow of Qi and Blood, tonifying where there is deficiency, draining where there is excess, and promoting free flow where there is stagnation. An axiom of the medical literature of acupuncture is "no pain, no blockage; no blockage, no pain."
Many patients claim to experience the sensations of stimulus known in Chinese as de qi ("obtaining the Qi" or "arrival of the Qi"). This kind of sensation was historically considered to be evidence of effectively locating the desired point. (There are some electronic devices now available which will make a noise when what they have been programmed to describe as the "correct" acupuncture point is pressed).
TCM treats the human body as a whole that involves several "systems of function" generally named after anatomical organs but not directly associated with them. The Chinese term for these systems is Zang Fu, where zang is translated as "viscera" or solid organs and fu is translated as "bowels" or hollow organs. In order to distinguish systems of function from physical organs, Zang Fu are capitalized in English, thus Lung, Heart, Kidney, etc. Disease is understood as a loss of balance of Yin, Yang, Qi and Blood (which bears some resemblance to homeostasis). Treatment of disease is attempted by modifying the activity of one or more systems of function through the activity of needles, pressure, heat, etc. on sensitive parts of the body of small volume traditionally called "acupuncture points" in English, or "xue" (穴, cavities) in Chinese. This is referred to in TCM as treating "patterns of disharmony."
Acupuncture points and meridians
Most of the main acupuncture points are found on the "twelve main meridians" and two of the "eight extra meridians" (Du Mai and Ren Mai) a total of "fourteen channels", which are described in classical and traditional Chinese medical texts, as pathways through which Qi and "Blood" flow. There also exist "extra points" not belonging to any channel. Other tender points (known as "ashi points") may also be needled as they are believed to be where stagnation has gathered.
Treatment of acupuncture points may be performed along several layers of pathways, most commonly the twelve primary channels, or mai, located throughout the body. The first twelve channels correspond to systems of function: Lung, Large Intestine, Stomach, Spleen, Heart, Small Intestine, Bladder, Kidney, Pericardium, San Jiao (an intangible, also known as Triple Burner), Gall Bladder, and Liver. Other pathways include the Eight Extraordinary Pathways (Qi Jing Ba Mai), the Luo Vessels, the Divergents and the Sinew Channels. Ashi (tender) points are generally used for treatment of local pain.
Of the eight extraordinary pathways, only two have acupuncture points of their own: the Ren Mai and Du Mai, which are situated on the midline of the anterior and posterior aspects of the trunk and head respectively. The other six meridians are "activated" by using a master and couple point technique which involves needling the acupuncture points located on the twelve main meridians that correspond to the particular extraordinary pathway.
The twelve primary pathways run vertically, bilaterally, and symmetrically and every channel corresponds to and connects internally with one of the twelve Zang Fu ("organs"). This means that there are six yin and six yang channels. There are three yin and three yang channels on each arm, and three yin and three yang on each leg.
- The three yin channels of the hand (Lung, Pericardium, and Heart) begin on the chest and travel along the inner surface (mostly the anterior portion) of the arm to the hand.
- The three yang channels of the hand (Large intestine, San Jiao, and Small intestine) begin on the hand and travel along the outer surface (mostly the posterior portion) of the arm to the head.
- The three yin channels of the foot (Spleen, Liver, and Kidney) begin on the foot and travel along the inner surface (mostly posterior and medial portion) of the leg to the chest or flank.
- The three yang channels of the foot (Stomach, Gallbladder, and Urinary Bladder) begin on the face, in the region of the eye, and travel down the body and along the outer surface (mostly the anterior and lateral portion) of the leg to the foot.
The movement of Qi through each of the twelve channels comprises an internal and an external pathway. The external pathway is what is normally shown on an acupuncture chart and is relatively superficial. All of the acupuncture points of a channel lie on its external pathway. The internal pathways are the deep course of the channel where it enters the body cavities and related Zang Fu organs. The superficial pathways of the twelve channels describe three complete circuits of the body, chest to hands, hands to head, head to feet, feet to chest, etc.
The distribution of Qi through the pathways is said to be as follows (the based on the demarcations in TCM's Chinese Clock): Lung channel of hand taiyin to Large Intestine channel of hand yangming to Stomach channel of foot yangming to Spleen channel of foot taiyin to Heart channel of hand shaoyin to Small Intestine channel of hand taiyang to Bladder channel of foot taiyang to Kidney channel of foot shaoyin to Pericardium channel of hand jueyin to San Jiao channel of hand shaoyang to Gallbladder channel of foot shaoyang to Liver channel of foot jueyin then back to the Lung channel of hand taiyin. According to the "Chinese clock", each channel occupies two hours, beginning with the Lung, 3AM-5AM, and coming full circle with the Liver 1AM-3AM.
A standard teaching text comments on the nature and relationship of meridians (or channels) and the Zang Fu organs:
- "The theory of the channels is interrelated with the theory of the Organs. Traditionally, the internal Organs have never been regarded as independent anatomical entities. Rather, attention has centered upon the functional and pathological interrelationships between the channel network and the Organs. So close is this identification that each of the twelve traditional Primary channels bears the name of one or another of the vital Organs.
- "In the clinic, the entire framework of diagnostics, therapeutics and point selection is based upon the theoretical framework of the channels. "It is because of the twelve Primary channels that people live, that disease is formed, that people are treated and disease arises." [(Spiritual Axis, chapter 12)]. From the beginning, however, we should recognize that, like other aspects of traditional medicine, channel theory reflects the limitations in the level of scientific development at the time of its formation, and is therefore tainted with the philosophical idealism and metaphysics of its day. That which has continuing clinical value needs to be reexamined through practice and research to determine its true nature.[7]
Traditional diagnosis
The acupuncturist decides which points to treat by observing and questioning the patient in order to make a diagnosis according to the tradition which he or she utilizes. In TCM, there are four diagnostic methods: inspection, auscultation and olfaction, inquiring, and palpation (Cheng, 1987, ch. 12).
- Inspection focuses on the face and particularly on the tongue, including analysis of the tongue size, shape, tension, color and coating, and the absence or presence of teeth marks around the edge.
- Auscultation and olfaction refer, respectively, to listening for particular sounds (such as wheezing) and attending to body odor.
- Inquiring focuses on the "seven inquiries", which are: chills and fever; perspiration; appetite, thirst and taste; defecation and urination; pain; sleep; and menses and leukorrhea.
- Palpation includes feeling the body for tender "ashi" points, and palpation of the left and right radial pulses at two levels of pressure (superficial and deep) and three positions Cun, Guan, Chi(immediately proximal to the wrist crease, and one and two fingers' breadth proximally, usually palpated with the index, middle and ring fingers).
Other forms of acupuncture employ additional diagnosic techniques. In many forms of classical Chinese acupuncture, as well as Japanese acupuncture, palpation of the muscles and the hara (abdomen) are central to diagnosis.
TCM perspective on treatment of disease
Although TCM is based on the treatment of "patterns of disharmony" rather than biomedical diagnoses, practitioners familiar with both systems have commented on relationships between the two. A given TCM pattern of disharmony may be reflected in a certain range of biomedical diagnoses: thus, the pattern called Deficiency of Spleen Qi could manifest as chronic fatigue, diarrhea or uterine prolapse. Likewise, a population of patients with a given biomedical diagnosis may have varying TCM patterns. These observations are encapsulated in the TCM aphorism "One disease, many patterns; one pattern, many diseases". (Kaptchuk, 1982)
Classically, in clinical practice, acupuncture treatment is typically highly individualized and based on philosophical constructs as well as subjective and intuitive impressions, and not on controlled scientific research.[24]
Criticism of TCM theory
TCM theory predates use of the scientific method and has received various criticisms based on scientific reductionist thinking, since there is no physically verifiable anatomical or histological basis for the existence of acupuncture points or meridians.
Felix Mann, founder and past-president of the Medical Acupuncture Society (1959–1980), the first president of the British Medical Acupuncture Society (1980), and the author of the first comprehensive English language acupuncture textbook Acupuncture: The Ancient Chinese Art of Healing' first published in 1962, has stated in his book Reinventing Acupuncture: A New Concept of Ancient Medicine:
- "The traditional acupuncture points are no more real than the black spots a drunkard sees in front of his eyes." (p. 14)
and…
- "The meridians of acupuncture are no more real than the meridians of geography. If someone were to get a spade and tried to dig up the Greenwich meridian, he might end up in a lunatic asylum. Perhaps the same fate should await those doctors who believe in [acupuncture] meridians." (p. 31)[5]
A report for CSICOP on pseudoscience in China written by Wallace Sampson and Barry Beyerstein said:
- "A few Chinese scientists we met maintained that although Qi is merely a metaphor, it is still a useful physiological abstraction (e.g., that the related concepts of Yin and Yang parallel modern scientific notions of endocrinologic and metabolic feedback mechanisms). They see this as a useful way to unite Eastern and Western medicine. Their more hard-nosed colleagues quietly dismissed Qi as only a philosophy, bearing no tangible relationship to modern physiology and medicine."[25]
George A. Ulett, MD, PhD, Clinical Professor of Psychiatry, University of Missouri School of Medicine states:
- "Devoid of metaphysical thinking, acupuncture becomes a rather simple technique that can be useful as a nondrug method of pain control." He believes that the traditional Chinese variety is primarily a placebo treatment, but electrical stimulation of about 80 acupuncture points has been proven useful for pain control."[26]
Ted J. Kaptchuk, author of The Web That Has No Weaver, refers to acupuncture as "prescientific." Regarding TCM theory, Kaptchuk states:
- "These ideas are cultural and speculative constructs that provide orientation and direction for the practical patient situation. There are few secrets of Oriental wisdom buried here. When presented outside the context of Chinese civilization, or of practical diagnosis and therapeutics, these ideas are fragmented and without great significance. The "truth" of these ideas lies in the way the physician can use them to treat real people with real complaints." (1983, pp. 34-35)
According to the 1997 NIH consensus statement on acupuncture:
- "Despite considerable efforts to understand the anatomy and physiology of the "acupuncture points", the definition and characterization of these points remains controversial. Even more elusive is the basis of some of the key traditional Eastern medical concepts such as the circulation of Qi, the meridian system, and the five phases theory, which are difficult to reconcile with contemporary biomedical information but continue to play an important role in the evaluation of patients and the formulation of treatment in acupuncture."[6]
Clinical practice

Most modern acupuncturists use disposable stainless steel needles of fine diameter (0.007" to 0.020", 0.18 mm to 0.51 mm), sterilized with ethylene oxide or by autoclave. These needles are far smaller in diameter (and therefore less painful) than the needles used to give shots, since they do not have to be hollow for purposes of injection. The upper third of these needles is wound with a thicker wire (typically bronze), or covered in plastic, to stiffen the needle and provide a handle for the acupuncturist to grasp while inserting. The size and type of needle used, and the depth of insertion, depend on the acupuncture style being practised.
Warming an acupuncture point, typically by moxibustion (the burning of a combination of herbs, primarily mugwort), is a different treatment than acupuncture itself and is often, but not exclusively, used as a supplemental treatment. The Chinese term zhēn jǐu (針灸), commonly used to refer to acupuncture, comes from zhen meaning "needle", and jiu meaning "moxibustion". Moxibustion is used to varying degrees among current schools of oriental medicine. For example, one well-known technique is to insert the needle at the desired acupuncture point, attach dried moxa to the external end of an acupuncture needle, and then ignite it. The moxa will then smolder for several minutes (depending on the amount adhered to the needle) and conduct heat through the needle to the tissue surrounding the needle in the patient's body. Another common technique is to hold a large glowing stick of moxa over the needles. Moxa is also sometimes burned at the skin surface, usually by applying an ointment to the skin to protect from burns, though burning of the skin is general practice in China.
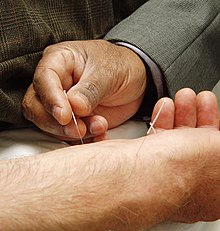
An example of acupuncture treatment
In Western medicine, vascular headaches (the kind that are accompanied by throbbing veins in the temples) are typically treated with analgesics such as aspirin and/or by the use of agents such as niacin that dilate the affected blood vessels in the scalp, but in acupuncture a common treatment for such headaches is to stimulate the sensitive points that is located roughly in the centers of the webs between the thumbs and the palms of the patient's hands, the hé gǔ points. These points are described by acupuncture theory as "targeting the face and head" and are considered to be the most important points when treating disorders affecting the face and head. The patient reclines, and the points on each hand are first sterilized with alcohol, and then thin, disposable needles are inserted to a depth of approximately 3-5 mm until a characteristic "twinge" is felt by the patient, often accompanied by a slight twitching of the area between the thumb and hand. Most patients report a pleasurable "tingling" sensation and feeling of relaxation while the needles are in place. The needles are retained for 15-20 minutes while the patient rests, and then are removed.
In the clinical practice of acupuncturists, patients frequently report one or more of certain kinds of sensation that are associated with this treatment:
- Extreme sensitivity to pain at the points in the webs of the thumbs.
- In bad headaches, a feeling of nausea that persists for roughly the same period as the stimulation being administered to the webs of the thumbs.
- Simultaneous relief of the headache. (See Zhen Jiu Xue, p. 177f et passim.)
Indications according to acupuncturists in the West
According to the American Academy of Medical Acupuncture (2004), acupuncture may be considered as a complementary therapy for the conditions in the list below.[27]
The conditions labeled with * are also included in the World Health Organization list of acupuncture indications.[28] These cases are based on clinical experience and are not necessarily substantiated by controlled clinical research. The inclusion of specific diseases is not meant to indicate the extent of acupuncture's efficacy in treating them.[28]
- Abdominal distention/flatulence*
- Acute and chronic pain control*
- Allergic sinusitis *
- Anesthesia for high-risk patients or patients with previous adverse responses to anesthetics
- Anorexia
- Anxiety, fright, panic*
- Arthritis/arthrosis *
- Atypical chest pain (negative workup)
- Bursitis, tendinitis, carpal tunnel syndrome*
- Certain functional gastrointestinal disorders (nausea and vomiting, esophageal spasm, hyperacidity, irritable bowel) *
- Cervical and lumbar spine syndromes*
| class="col-break " |
- Constipation, diarrhea *
- Cough with contraindications for narcotics
- Drug detoxification *
- Dysmenorrhea, pelvic pain *
- Frozen shoulder *
- Headache (migraine and tension-type), vertigo (Meniere disease), tinnitus *
- Idiopathic palpitations, sinus tachycardia
- In fractures, assisting in pain control, edema, and enhancing healing process
- Muscle spasms, tremors, tics, contractures*
- Neuralgias (trigeminal, herpes zoster, postherpetic pain, other)
- Paresthesias *
- Persistent hiccups*
- Phantom pain
| class="col-break " |
- Plantar fasciitis*
- Post-traumatic and post-operative ileus *
- Premenstrual syndrome[29]
- Selected dermatoses (urticaria, pruritus, eczema, psoriasis)
- Sequelae of stroke syndrome (aphasia, hemiplegia) *
- Seventh nerve palsy
- Severe hyperthermia
- Sleep disorders[30]
- Sprains and contusions
- Temporo-mandibular joint derangement, bruxism *
- Urinary incontinence, retention (neurogenic, spastic, adverse drug effect) *
- Weight Loss
Scientific theories and mechanisms of action
Many hypotheses have been proposed to address the physiological mechanisms of action of acupuncture.[31]
Gate-control theory of pain
The "gate control theory of pain" (developed by Ronald Melzack and Patrick Wall in 1962[32] and in 1965[33]) proposed that pain perception is not simply a direct result of activating pain fibers, but modulated by interplay between excitation and inhibition of the pain pathways. According to the theory, the "gating of pain" is controlled by the inhibitory action on the pain pathways. That is, the perception of pain can be altered (gated on or off) by a number of means physiologically, psychologically and pharmacologically. The gate-control theory was developed in neuroscience independent of acupuncture, which later was proposed as a mechanism to account for the hypothesized analgesic action of acupuncture in the brainstem reticular formation by a German neuroscientist in 1976.[34]
This leads to the theory of central control of pain gating, i.e., pain blockade at the brain (i.e., central to the brain rather than at the spinal cord or periphery) via the release of endogenous opioid (natural pain killers in the brain) neurohormones, such as endorphins and enkephalins (naturally occurring morphines).
Neurohormonal theory

Pain transmission can also be modulated at many other levels in the brain along the pain pathways, including the periaqueductal gray, thalamus, and the feedback pathways from the cerebral cortex back to the thalamus. Pain blockade at these brain locations is often mediated by neurohormones, especially those that bind to the opioid receptors (pain-blockade site).
Some studies suggest that the analgesic (pain-killing) action of acupuncture is associated with the release of natural endorphins in the brain. This effect can be inferred by blocking the action of endorphins (or morphine) using a drug called naloxone. When naloxone is administered to the patient, the analgesic effects of morphine can be reversed, causing the patient to feel pain again. When naloxone is administered to an acupunctured patient, the analgesic effect of acupuncture can also be reversed, causing the patient to report an increased level of pain.[35][36][37][38] It should be noted, however, that studies using similar procedures, including the administration of naloxone, have suggested a role of endogenous opioids in the placebo response, demonstrating that this response is not unique to acupuncture.[39]
One study performed on monkeys by recording the neural activity directly in the thalamus of the brain indicated that acupuncture's analgesic effect lasted more than an hour.[40] Furthermore, there is a large overlap between the nervous system and acupuncture trigger points (points of maximum tenderness) in myofascial pain syndrome.[41]
Evidence suggests that the sites of action of analgesia associated with acupuncture include the thalamus using fMRI (functional magnetic resonance imaging)[42] and PET (positron emission tomography)[43] brain imaging techniques,[44] and via the feedback pathway from the cerebral cortex using electrophysiological recording of the nerve impulses of neurons directly in the cortex, which shows inhibitory action when acupuncture stimulus is applied.[45] Similar effects have been observed in association with the placebo response. One study using fMRI found that placebo analgesia was associated with decreased activity in the thalamus, insula and anterior cingulate cortex.[46]
Recently, acupuncture has been shown to increase the nitric oxide levels in treated regions, resulting in increased local blood circulation.[47][48] Effects on local inflammation and ischemia have also been reported.[49]
Issues in study design
One of the major challenges in acupuncture research is in the design of an appropriate placebo control group.[50] In trials of new drugs, double blinding is the accepted standard, but since acupuncture is a procedure rather than a pill, it is difficult to design studies in which both the acupuncturist and patient are blinded as to the treatment being given. The same problem arises in double-blinding procedures used in biomedicine, including virtually all surgical procedures, dentistry, physical therapy, etc.
Blinding of the practitioner in acupuncture remains challenging. One proposed solution to blinding patients has been the development of "sham acupuncture", i.e., needling performed superficially or at non-acupuncture sites. Controversy remains over whether, and under what conditions, sham acupuncture may function as a true placebo, particularly in studies on pain, in which insertion of needles anywhere near painful regions may elicit a beneficial response.[51][6] A review in 2007 noted several issues confounding sham acupuncture:
Weak physiologic activity of superficial or sham needle penetration is suggested by several lines of research, including RCTs showing larger effects of a superficial needle penetrating acupuncture than those of a nonpenetrating sham control, positron emission tomography research indicating that sham acupuncture can stimulate regions of the brain associated with natural opiate production, and animal studies showing that sham needle insertion can have nonspecific analgesic effects through a postulated mechanism of “diffuse noxious inhibitory control”. Indeed, superficial needle penetration is a common technique in many authentic traditional Japanese acupuncture styles.[52]
A study by Ted Kaptchuk et. al. showed that sham acupuncture exerted a stronger effect on pain than an inert pill did, and concluded: "Placebo effects seem to be malleable and depend on the behaviours embedded in medical rituals."[53]
Scientific research into efficacy
Evidence-based medicine
There is scientific agreement that an evidence-based medicine (EBM) framework should be used to assess health outcomes and that systematic reviews with strict protocols are essential. Organizations such as the Cochrane Collaboration and Bandolier publish such reviews. In practice, EBM is "about integrating individual clinical expertise and the best external evidence" and thus does not demand that doctors ignore research outside its "top-tier" criteria.[54]
The development of the evidence base for acupuncture was summarized in a review by researcher Edzard Ernst and colleagues in 2007. They compared systematic reviews conducted (with similar methodology) in 2000 and 2005:
- The effectiveness of acupuncture remains a controversial issue. ... The results indicate that the evidence base has increased for 13 of the 26 conditions included in this comparison. For 7 indications it has become more positive (i.e. favoring acupuncture) and for 6 it had changed in the opposite direction. It is concluded, that acupuncture research is active. The emerging clinical evidence seems to imply that acupuncture is effective for some but not all conditions.[11]
For low back pain, a Cochrane review (2005) stated:
- Thirty-five RCTs covering 2861 patients were included in this systematic review. There is insufficient evidence to make any recommendations about acupuncture or dry-needling for acute low-back pain. For chronic low-back pain, results show that acupuncture is more effective for pain relief than no treatment or sham treatment, in measurements taken up to three months. The results also show that for chronic low-back pain, acupuncture is more effective for improving function than no treatment, in the short-term. Acupuncture is not more effective than other conventional and "alternative" treatments. When acupuncture is added to other conventional therapies, it relieves pain and improves function better than the conventional therapies alone. However, effects are only small. Dry-needling appears to be a useful adjunct to other therapies for chronic low-back pain.[55]
A 2008 study suggest that combining acupuncture with conventional infertility treatments such as IVF greatly improves the success rates of such medical interventions.[56]
A review by Manheimer et al. in Annals of Internal Medicine (2005) reached conclusions similar to Cochrane's review on low back pain.[57] A review for the American Pain Society/American College of Physicians found fair evidence that acupuncture is effective for chronic low back pain.[58]
For nausea[59] and vomiting: The Cochrane review (Lee and Done, 2006) on the use of the P6 acupoint for the reduction of post-operative nausea and vomiting concluded that the use of P6 acupoint stimulation can reduce the risk of postoperative nausea and vomiting with minimal side effects, albeit with efficacy less than or equal to prophylactic (i.e., preventative) treatment with antiemetic drugs.[60][61] Cochrane also stated: "Electroacupuncture is effective for first day vomiting after chemotherapy, but trials considering modern antivomiting drugs are needed."[62]
A 2007 Cochrane Review for the use of acupuncture for neck pain stated:
- There is moderate evidence that acupuncture relieves pain better than some sham treatments, measured at the end of the treatment. There is moderate evidence that those who received acupuncture reported less pain at short term follow-up than those on a waiting list. There is also moderate evidence that acupuncture is more effective than inactive treatments for relieving pain post-treatment and this is maintained at short-term follow-up.[63]
For headache, Cochrane concluded (2006) that "(o)verall, the existing evidence supports the value of acupuncture for the treatment of idiopathic headaches. However, the quality and amount of evidence are not fully convincing. There is an urgent need for well-planned, large-scale studies to assess the effectiveness and cost-effectiveness of acupuncture under real-life conditions."[64]
For osteoarthritis, reviews since 2006 show a trivial difference between sham and true acupuncture.[52][65]
For fibromyalgia, a systematic review of the best 5 randomized controlled trials available found mixed results.[66] Three positive studies, all using electro-acupuncture, found short term benefits. The methodological quality of the 5 trials was mixed and frequently low.
For the following conditions, the Cochrane Collaboration has concluded there is insufficient evidence to determine whether acupuncture is beneficial, often because of the paucity and poor quality of the research, and that further research is needed:
- Chronic asthma[67]
- Bell's palsy[68]
- Cocaine dependence (auricular acupuncture)[69]
- Depression[70]
- Primary dysmenorrhoea (acupuncture plus transcutaneous electrical nerve stimulation)[71]
- Epilepsy[72]
| class="col-break " |
- Glaucoma[73]
- Insomnia[74]
- Irritable bowel syndrome[75]
- Induction of childbirth[76]
- Rheumatoid arthritis[77]
- Shoulder pain[78]
| class="col-break " |
- Schizophrenia[79]
- Smoking cessation[80]
- Acute stroke[81]
- Stroke rehabilitation[82]
- Tennis elbow (lateral elbow pain)[83]
- Vascular dementia[84]
Positive results from some studies on the efficacy of acupuncture may be as a result of poorly designed studies or publication bias.[85][86]
Evidence from neuroimaging studies
Acupuncture appears to have effects on cortical activity, as demonstrated by magnetic resonance imaging and positron emission tomography. A 2005 literature review[87] concluded that neuroimaging data to date show some promise for being able to distinguish the effects of expectation, placebo, and real acupuncture. The studies reviewed were mostly small and pain-related, and more research is needed to determine the specificity of neural substrate activation in non-painful indications.
NIH consensus statement
In 1997, the National Institutes of Health (NIH) issued a consensus statement on acupuncture that concluded that
- there is sufficient evidence of acupuncture's value to expand its use into conventional medicine and to encourage further studies of its physiology and clinical value.[6]
The statement was not a policy statement of the NIH but is the considered assessment of a panel convened by the NIH.
The NIH consensus statement said that
- the data in support of acupuncture are as strong as those for many accepted Western medical therapies
and added that
- there is clear evidence that needle acupuncture is efficacious for adult postoperative and chemotherapy nausea and vomiting and probably for the nausea of pregnancy... There is reasonable evidence of efficacy for postoperative dental pain... reasonable studies (although sometimes only single studies) showing relief of pain with acupuncture on diverse pain conditions such as menstrual cramps, tennis elbow, and fibromyalgia...
The NIH consensus statement summarized and made a prediction:
- Acupuncture as a therapeutic intervention is widely practiced in the United States. While there have been many studies of its potential usefulness, many of these studies provide equivocal results because of design, sample size, and other factors. The issue is further complicated by inherent difficulties in the use of appropriate controls, such as placebos and sham acupuncture groups. However, promising results have emerged, for example, showing efficacy of acupuncture in adult postoperative and chemotherapy nausea and vomiting and in postoperative dental pain. There are other situations such as addiction, stroke rehabilitation, headache, menstrual cramps, tennis elbow, fibromyalgia, myofascial pain, osteoarthritis, low back pain, carpal tunnel syndrome, and asthma, in which acupuncture may be useful as an adjunct treatment or an acceptable alternative or be included in a comprehensive management program. Further research is likely to uncover additional areas where acupuncture interventions will be useful.
The NIH's National Center for Complementary and Alternative Medicine continues to abide by the recommendations of the NIH Consensus Statement, stating that:
- Preclinical studies have documented acupuncture's effects, but they have not been able to fully explain how acupuncture works within the framework of the Western system of medicine that is commonly practiced in the United States.[12]
American Medical Association statement
In 1997, the following statement was adopted as policy of the American Medical Association (AMA), an association of medical doctors and medical students, after a report on a number of alternative therapies including acupuncture:[88]
"There is little evidence to confirm the safety or efficacy of most alternative therapies. Much of the information currently known about these therapies makes it clear that many have not been shown to be efficacious. Well-designed, stringently controlled research should be done to evaluate the efficacy of alternative therapies."
German study
A German study published in the September 2007 issue of the Archives of Internal Medicine found that nearly half of patients treated with acupuncture or a sham treatment felt relief from chronic low back pain over a period of months compared to just nearly a quarter of those receiving a variety of more conventional treatments (drugs, heat, massage, etc.)[89][90] The greater benefit of the real and sham treatments were not significantly different.
Nonacupuncture points
A controlled study of 300 migraine patients found that both sham and real acupuncture resulted in improvements compared with patients on a waiting list, with no significant difference in benefit between the sham and active treatment groups. The sham treatment involved actual needles piercing the skin, but at nonacupuncture points.[91]
Some researchers have questioned the use of sham acupuncture as a control in this study[92] and others, arguing that sham acupuncture may be too similar to real acupuncture to be a valid control, thereby skewing results toward showing a relative lack of efficacy.
Safety and risks
Because acupuncture needles penetrate the skin, many forms of acupuncture are invasive procedures, and therefore not without risk. Injuries are rare among patients treated by trained practitioners.[93][94] In most jurisdictions, needles are required by law to be sterile, disposable and used only once; in some places, needles may be reused if they are first resterilized, e.g. in an autoclave.
Several styles of Japanese acupuncture use non-inserted needling, making for an entirely non-invasive procedure. In non-inserted needling the needle is brought to the skin, but never penetrates it, and various other acupuncture tools are used to tap or stroke along the meridians. Notable examples of these styles are Tōyōhari and the pediatric acupuncture style Shōnishin.
Common, minor adverse events
A survey by Ernst et al. of over 400 patients receiving over 3500 acupuncture treatments found that the most common adverse effects from acupuncture were:[13]
- Minor bleeding after removal of the needles, seen in roughly 3% of patients. (Holding a cotton ball for about one minute over the site of puncture is usually sufficient to stop the bleeding.)
- Hematoma, seen in about 2% of patients, which manifests as bruises. These usually go away after a few days.
- Dizziness, seen in about 1% of patients. Some patients have a conscious or unconscious fear of needles which can produce dizziness and other symptoms of anxiety. Patients are usually treated lying down in order to reduce likelihood of fainting.
The survey concluded: "Acupuncture has adverse effects, like any therapeutic approach. If it is used according to established safety rules and carefully at appropriate anatomic regions, it is a safe treatment method."[13]
Other injury
Other risks of injury from the insertion of acupuncture needles include:
- Nerve injury, resulting from the accidental puncture of any nerve.
- Brain damage or stroke, which is possible with very deep needling at the base of the skull.
- Pneumothorax from deep needling into the lung.[95]
- Kidney damage from deep needling in the low back.
- Haemopericardium, or puncture of the protective membrane surrounding the heart, which may occur with needling over a sternal foramen (a hole in the breastbone that occurs as the result of a congenital defect.) [96]
- Risk of terminating pregnancy with the use of certain acupuncture points that have been shown to stimulate the production of adrenocorticotropic hormone (ACTH) and oxytocin.
The chance of these is very small; the risk can be further reduced through proper training of acupuncturists. Graduates of medical schools and (in the US) accredited acupuncture schools receive thorough instruction in proper technique so as to avoid these events. (Cf. Cheng, 1987)
Risks from omitting orthodox medical care
Receiving any form of alternative medical care without also receiving orthodox Western medical care can be inherently risky [citation needed] , since undiagnosed disease may go untreated and could worsen. For this reason many acupuncturists and doctors prefer to consider acupuncture a complementary therapy rather than an alternative therapy.
Critics also express concern that unethical or naive practitioners may induce patients to exhaust financial resources by pursuing ineffective treatment.[97][98] Some public health departments regulate acupuncture.[99][100][101]
Safety compared with other treatments
Commenting on the relative safety of acupuncture compared with other treatments, the NIH consensus panel stated that "(a)dverse side effects of acupuncture are extremely low and often lower than conventional treatments." They also stated:
- "the incidence of adverse effects is substantially lower than that of many drugs or other accepted medical procedures used for the same condition. For example, musculoskeletal conditions, such as fibromyalgia, myofascial pain, and tennis elbow... are conditions for which acupuncture may be beneficial. These painful conditions are often treated with, among other things, anti-inflammatory medications (aspirin, ibuprofen, etc.) or with steroid injections. Both medical interventions have a potential for deleterious side effects but are still widely used and are considered acceptable treatments."
In a Japanese survey of 55,291 acupuncture treatments given over five years by 73 acupuncturists, 99.8% of them were performed with no significant minor adverse effects and zero major adverse incidents (Hitoshi Yamashita, Bac, Hiroshi Tsukayama, BA, Yasuo Tanno, MD, PhD. Kazushi Nishijo, PhD, JAMA). Two combined studies in the UK of 66,229 acupuncture treatments yielded only 134 minor adverse events. (British Medical Journal 2001 Sep 1). The total of 121,520 treatments with acupuncture therapy were given with no major adverse incidents (for comparison, a single such event would have indicated a 0.0008% incidence).
Legal and political status
Acupuncturists may also practice herbal medicine or tui na, or may be medical acupuncturists, who, as well as being qualified physicians, also practice acupuncture in a simplified form. In most states, medical doctors are not required to have any formal training to perform acupuncture. Over 20 states allow chiropractors to perform acupuncture with less than 200 hours training. The typical amount of hours of medical training by licensed acupuncturists is over 3,000 hours. License is regulated by the state or province in many countries, and often requires passage of a board exam.
In the US, acupuncture is practiced by a variety of healthcare providers. Those who specialize in Acupuncture and Oriental Medicine are usually referred to as "licensed acupuncturists", or L.Ac.'s. The abbreviation "Dipl. Ac." stands for "Diplomate of Acupuncture" and signifies that the holder is board-certified by the NCCAOM[102]. Professional degrees are usually at the level of a Master's degree.
A poll of American doctors in 2005 showed that 59% believe acupuncture was at least somewhat effective.[103] In 1996, the Food and Drug Administration changed the status of acupuncture needles from Class III to Class II medical devices, meaning that needles are regarded as safe and effective when used appropriately by licensed practitioners.[104][105]
Canadian acupuncturists have been licensed in British Columbia since 2003. In Ontario, the practice of acupuncture is now regulated by the Traditional Chinese Medicine Act, 2006, S.o. 2006, chapter 27.[106] The government is in the process of establishing a College[107] whose mandate will be to oversee the implementation of policies and regulations relating to the profession.
In the United Kingdom, acupuncturists are not yet regulated by the government.
In Australia, the legalities of practicing acupuncture also vary by state. Victoria is the only state of Australia with an operational registration board.[108] Currently acupuncturists in New South Wales are bound by the guidelines in the Public Health (Skin Penetration) Regulation 2000,[109] which is enforced at local council level. Other states of Australia have their own skin penetration acts.
Many other countries do not license acupuncturists or require them be trained.
See also
- Acupoint therapy
- Acupressure
- Acupuncture detoxification
- Auriculotherapy
- Chin na
- Complementary and Alternative Medicine
- Dry needling
- Electroacupuncture
- Medical acupuncture
- Pressure Points
- Qi
- Qigong
- Seitai
- Susuk
- T'ai Chi Ch'uan
- Traditional Chinese medicine
- Trigger point
- Veterinary acupuncture
- Thought Field Therapy
- Emotional Freedom Technique
- Tapas Acupressure Technique
Bibliography
- Vincent CA, Richardson PH (1986). "The evaluation of therapeutic acupuncture: concepts and methods". Pain. 24 (1): 1–13. PMID 3513094.
- Richardson PH, Vincent CA (1986). "Acupuncture for the treatment of pain". Pain. 24: 1540. doi:10.1016/0304-3959(86)90023-0.
- Ter Riet G; et al. (1989). "The effectiveness of acupuncture". Huisarts Wet. 32: 170–175, 176–181, 308–312.
{{cite journal}}: Explicit use of et al. in:|author=(help) - Brinkhaus B, Hummelsberger J, Kohnen R; et al. (2004). "Acupuncture and Chinese herbal medicine in the treatment of patients with seasonal allergic rhinitis: a randomized-controlled clinical trial". Allergy. 59 (9): 953–60. doi:10.1111/j.1398-9995.2004.00540.x. PMID 15291903.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - Cheng Xinnong. Chinese Acupuncture and Moxibustion, First Edition (1987), Fourth Printing (1996. Foreign Languages Press, First ed., 1987. ISBN 7-119-00378-X
- G. Maciocia. The Foundations of Chinese Medicine: A Comprehensive Text for Acupuncturists and Herbalists. Second Edition. Churchill Livingstone. 1989
- P. Deadman, K. Baker, M. Al-Khafaji. A Manual of Acupuncture. Eastland Press
- Witt C, Brinkhaus B, Jena S; et al. (2005). "Acupuncture in patients with osteoarthritis of the knee: a randomised trial". Lancet. 366 (9480): 136–43. doi:10.1016/S0140-6736(05)66871-7. PMID 16005336.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - Edwards, J. Acupuncture and Heart Health. Access, February 2002
- Wolfe HL (August/September 2005). "Chronic Fatigue Syndrome, Acupuncture and its related modalities" (Reprint at findarticles.com). Townsend Letter for Doctors and Patients.
{{cite web}}: Check date values in:|date=(help) - Abuaisha BB, Costanzi JB, Boulton AJ (1998). "Acupuncture for the treatment of chronic painful peripheral diabetic neuropathy: a long-term study". Diabetes Res. Clin. Pract. 39 (2): 115–21. PMID 9597381.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - Altshul, Sara. "Incontinence: Finally, Relief That Works." Prevention December 2005: 33. Academic Search Premier. EBSCO. 30 January 2006
- Deluze C, Bosia L, Zirbs A, Chantraine A, Vischer TL (1992). "Electroacupuncture in fibromyalgia: results of a controlled trial". BMJ. 305 (6864): 1249–52. PMID 1477566.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - Cademartori, Lorraine. "Facing the Point." Forbes October 2005: 85. Academic Search
- Ouyang H, Chen JD (2004). "Review article: therapeutic roles of acupuncture in functional gastrointestinal disorders". Aliment. Pharmacol. Ther. 20 (8): 831–41. doi:10.1111/j.1365–2036.2004.02196.x. PMID 15479354.
{{cite journal}}: Check|doi=value (help) - Teng, Liang-yüeh; Chʻeng, Hsin-nung (1987). Chinese acupuncture and moxibustion. Beijing: Foreign Language Press. ISBN 7-119-00378-X.
{{cite book}}: CS1 maint: multiple names: authors list (link) - Helms JM (1987). "Acupuncture for the management of primary dysmenorrhea". Obstetrics and gynecology. 69 (1): 51–6. PMID 3540764.
- Jin, Guanyuan, Xiang, Jia-Jia and Jin, Lei: Clinical Reflexology of Acupuncture and Moxibustion (Chinese). Beijing Science and Technology Press, Beijing, 2004. ISBN 7-5304-2862-4
- Jin, Guan-Yuan, Jin, Jia-Jia X. and Jin, Louis L.: Contemporary Medical Acupuncture - A Systems Approach (English). Springer, USA & Higher Education Press, PRC, 2006. ISBN 7-04-019257-8
- Kaptchuk, Ted J. (1983). The web that has no weaver: understanding Chinese medicine. New York, N.Y: Congdon & Weed. ISBN 0-86553-109-9.
- Premier. EBSCO. 30 January 2006
- "History of Acupuncture in China." Acupuncture Care. 2 February 2006 <http://www.acupuncturecare.com/acupunct.htm>
- Howard, Cori. "An Ancient Helper for Making a Baby." Maclean’s 23 January 2006: 40. Academic Search Premier. EBSCO. 30 January 2006
- Carter B (2007-07-04). "Is Acupuncture Safe?". ArticlesLog.com. Retrieved 2007-07-20.
- Health Professions Regulatory Advisory Council, Minister’s Referral Letter January 18, 2006 – Traditional Chinese Medicine (TCM) <http://www.hprac.org/english/projects.asp> 20 March 2006
- Porkert, Manfred (1974). The theoretical foundations of Chinese medicine: systems of correspondence. Cambridge, Mass: MIT Press. ISBN 0-262-16058-7.
- Wu MT, Hsieh JC, Xiong J; et al. (1999). "Central nervous pathway for acupuncture stimulation: localization of processing with functional MR imaging of the brain--preliminary experience". Radiology. 212 (1): 133–41. PMID 10405732.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link)
Footnotes
- ^ Whole Medical Systems: An Overview [NCCAM Backgrounder]
- ^ Energy Medicine: An Overview [NCCAM Backgrounder]
- ^ ABC Chinese-English Comprehensive Dictionary edited by John DeFrancis, as used in Wenlin version 3.4.1
- ^ Acupuncture: the Chinese practice of piercing specific areas of the body along peripheral nerves with fine needles to relieve pain, induce surgical anesthesia, and for therapeutic purposes. Dorland's Pocket Medical Dictionary, 25th ed. W. B. Saunders Co., 1995. ISBN 0-7216-5738-9
- ^ a b Felix Mann. Chinese Medicine Times, vol 1 issue 4, Aug. 2006, "The Final Days of Traditional Beliefs? - Part One" Cite error: The named reference "Mann F." was defined multiple times with different content (see the help page).
- ^ a b c d e f NIH Consensus Development Program (November 3–5, 1997). "Acupuncture --Consensus Development Conference Statement". National Institutes of Health. Retrieved 2007-07-17.
{{cite web}}: CS1 maint: date format (link) - ^ a b Acupuncture: A Comprehensive Text, p. 35. Shanghai College of Traditional Chinese Medicine. Translated and edited by John O'Connor and Dan Bensky. Eastland Press, Seattle, 1981 (Fourteenth Printing, 1997). ISBN 0-939616-00-9.
- ^ Cheng Xinnong. Chinese Acupuncture and Moxibustion, p. 53. Foreign Languages Press, 1987 (First edition; Fourth Printing, 1996). ISBN 7-119-00378-X
- ^ Kaptchuk, The Web That Has No Weaver, 1983, pp. 34-35
- ^ Ernst, Edzard (2006-02). "Acupuncture - a critical analysis". Journal of Internal Medicine. 259 (2): 125–137. doi:10.1111/j.1365–2796.2005.01584.x. PMID 16420542. Retrieved 2008-04-08.
{{cite journal}}: Check|doi=value (help); Check date values in:|date=(help) - ^ a b Ernst E, Pittler MH, Wider B, Boddy K. (2007). "Acupuncture: its evidence-base is changing". Am J Chin Med. 35 (1): 21–5. doi:10.1142/S0192415X07004588. PMID 17265547.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ a b "Get the Facts, Acupuncture". National Institute of Health. 2006. Retrieved 2006-03-02.
- ^ a b c Ernst G, Strzyz H, Hagmeister H (2003). "Incidence of adverse effects during acupuncture therapy-a multicentre survey". Complementary therapies in medicine. 11 (2): 93–7. PMID 12801494.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ MoonDragon's Health & Wellness Therapy: Acupuncture
- ^ Acupuncture
- ^ http://www.ogka.at/a_p_oetzi.asp?nav_reihenfolge=9
- ^ Elsevier
- ^ http://www.redwingbooks.com/html/catalog/index.cfm/action_search/type_detail/InventoryKey_UndAcu/file_Chapter
- ^ History Of Acupuncture
- ^ Unschuld, Paul. Chinese Medicine, p. 94. 1998, Paradigm Publications
- ^ a b c d e f Scott Suvow. "History of Acupuncture in China". Acupuncture Care. Retrieved 2008-09-02.
- ^ Acupuncture Anaesthesia And the Physiological Basis of Acupuncture: Acupuncture Anaesthesia - George T. Lewith M.A., M.R.C.G.P., M.R.C.P. - HealthWorld Online
- ^ http://www.acupunctureflorida.com/sacr.html
- ^ Medical Acupuncture - Spring / Summer 2000- Volume 12 / Number 1
- ^ Sampson, Wallace Sampson (1996). "Traditional Medicine and Pseudoscience in China: A Report of the Second CSICOP Delegation (Part 2)". Skeptical Inquirer. 20 (5). Retrieved 2007-01-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|month=ignored (help) - ^ Ulett GA, Acupuncture update 1984, Southern Medical Journal 78:233234, 1985. Comment found at NCBI - Traditional and evidence-based acupuncture: history, mechanisms, and present status. Ulett GA, Han J, Han S.
- ^ Braverman S (2004). "Medical Acupuncture Review: Safety, Efficacy, And Treatment Practices". Medical Acupuncture. 15 (3).
- ^ a b The World Health Organization Viewpoint On Acupuncture
- ^ Proctor ML, Smith CA, Farquhar CM, Stones RW (2002). "Transcutaneous electrical nerve stimulation and acupuncture for primary dysmenorrhoea". Cochrane Database Syst Rev (1): CD002123. PMID 11869624.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Gooneratne NS (2008). "Complementary and alternative medicine for sleep disturbances in older adults". Clin. Geriatr. Med. 24 (1): 121–38, viii. doi:10.1016/j.cger.2007.08.002. PMID 18035236.
- ^ MedlinePlus: Acupuncture
- ^ P.D. Wall, R. Melzack, On nature of cutaneous sensory mechanisms, Brain, 85:331, 1962.
- ^ R. Melzack, P.D. Wall, Pain mechanisms: A new theory, Science, 150:171-9, 1965.
- ^ Melzack R. Acupuncture and pain mechanisms Anaesthesist. 1976;25:204-7.
- ^ Pomeranz B, Chiu D (1976). "Naloxone blockade of acupuncture analgesia: endorphin implicated". Life Sci. 19 (11): 1757–62. PMID 187888.
- ^
Mayer DJ, Price DD, Rafii A (1977). "Antagonism of acupuncture analgesia in man by the narcotic antagonist naloxone". Brain Res. 121 (2): 368–72. PMID 832169.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Eriksson SV, Lundeberg T, Lundeberg S (1991). "Interaction of diazepam and naloxone on acupuncture induced pain relief". Am. J. Chin. Med. 19 (1): 1–7. PMID 1654741.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Bishop B. - Pain: its physiology and rationale for management. Part III. Consequences of current concepts of pain mechanisms related to pain management. Phys Ther. 1980, 60:24-37.
- ^ Amanzio, M., Pollo, A., Maggi, G., Benedetti, F. (2001). "Response Variability to Analgesics: a Role for Non-specific Activation of Endogenous Opioids". Pain. 90 (3): 205–215.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Sandrew BB, Yang RC, Wang SC (1978). "Electro-acupuncture analgesia in monkeys: a behavioral and neurophysiological assessment". Archives internationales de pharmacodynamie et de thérapie. 231 (2): 274–84. PMID 417686.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Melzack R, Stillwell DM, Fox EJ (1977). "Trigger points and acupuncture points for pain: correlations and implications". Pain. 3 (1): 3–23. PMID 69288.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Li K, Shan B, Xu J; et al. (2006). "Changes in FMRI in the human brain related to different durations of manual acupuncture needling". Journal of alternative and complementary medicine (New York, N.Y.). 12 (7): 615–23. doi:10.1089/acm.2006.12.615. PMID 16970531.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Pariente J, White P, Frackowiak RS, Lewith G (2005). "Expectancy and belief modulate the neuronal substrates of pain treated by acupuncture". Neuroimage. 25 (4): 1161–7. doi:10.1016/j.neuroimage.2005.01.016. PMID 15850733.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Shen J (2001). "Research on the neurophysiological mechanisms of acupuncture: review of selected studies and methodological issues". Journal of alternative and complementary medicine (New York, N.Y.). 7 Suppl 1: S121–7. doi:10.1089/107555301753393896. PMID 11822627.
- ^ Liu JL, Han XW, Su SN (1990). "The role of frontal neurons in pain and acupuncture analgesia". Sci. China, Ser. B, Chem. Life Sci. Earth Sci. 33 (8): 938–45. PMID 2242217.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Wagner, T.D., Rilling, J.K., Smith, E.E., Sokolik, A., Casey, K.L.; et al. (2007). "Placebo-Induced Changes in fMRI in the Anticipation and Experience of Pain". Science. 303 (5661): 1162–1167.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Tsuchiya M, Sato EF, Inoue M, Asada A (2007). "Acupuncture enhances generation of nitric oxide and increases local circulation". Anesth. Analg. 104 (2): 301–7. doi:10.1213/01.ane.0000230622.16367.fb. PMID 17242084.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Blom M, Lundeberg T, Dawidson I, Angmar-Månsson B (1993). "Effects on local blood flux of acupuncture stimulation used to treat xerostomia in patients suffering from Sjögren's syndrome". Journal of oral rehabilitation. 20 (5): 541–8. PMID 10412476.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Lundeberg T (1993). "Peripheral effects of sensory nerve stimulation (acupuncture) in inflammation and ischemia". Scandinavian journal of rehabilitation medicine. Supplement. 29: 61–86. PMID 8122077.
- ^ White AR, Filshie J, Cummings TM (2001). "Clinical trials of acupuncture: consensus recommendations for optimal treatment, sham controls and blinding". Complement Ther Med. 9 (4): 237–245. PMID 12184353.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Johnson MI (2006). "The clinical effectiveness of acupuncture for pain relief--you can be certain of uncertainty". Acupunct Med. 24 (2): 71–9. PMID 16783282.
- ^ a b Meta-analysis: acupuncture for osteoarthritis of the knee. Eric Manheimer, Klaus Linde, Lixing Lao, Lex M Bouter, Brian M Berman. Ann Intern Med. 2007 Jun 19;146 (12):868-77. Full text (PDF)
- ^ Kaptchuk et. al., BMJ 2006;332:391-397
- ^ [http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=32159 Message to complementary and alternative medicine: evidence is a better friend than power. Andrew J Vickers]
- ^ Furlan AD, van Tulder MW, Cherkin DC; et al. (2005). "Acupuncture and dry-needling for low back pain". Cochrane database of systematic reviews (Online) (1): CD001351. doi:10.1002/14651858.CD001351.pub2. PMID 15674876.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Manheimer E, Zhang G, Udoff L, Haramati A, Langenberg P, Berman BM, Bouter LM (2008). "Effects of acupuncture on rates of pregnancy and live birth among women undergoing in vitro fertilisation: systematic review and meta-analysis". BMJ. 336 (7643): 545–9. PMID 18258932.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Manheimer E, White A, Berman B, Forys K, Ernst E (2005). "Meta-analysis: acupuncture for low back pain" (PDF). Ann. Intern. Med. 142 (8): 651–63. PMID 15838072.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Chou R, Huffman LH (2007). "Nonpharmacologic therapies for acute and chronic low back pain: a review of the evidence for an American Pain Society/American College of Physicians clinical practice guideline". Ann Intern Med. 147 (7): 492–504. doi:10.1001/archinte.147.3.492. PMID 17909210.
- ^ Dibble SL, Luce J, Cooper BA, Israel J, Cohen M, Nussey B, Rugo H (2007). "Acupressure for chemotherapy-induced nausea and vomiting: a randomized clinical trial". Oncol Nurs Forum. 34 (4): 813–20. doi:10.1188/07.ONF.xxx-xxx. PMID 17723973.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Lee A, Done ML (2004). "Stimulation of the wrist acupuncture point P6 for preventing postoperative nausea and vomiting". Cochrane database of systematic reviews (Online) (3): CD003281. doi:10.1002/14651858.CD003281.pub2. PMID 15266478.
- ^ For nausea, acupuncture at first appeared to be more effective than antiemetic drugs, per Lee and Done (2006); however, the authors later retracted this conclusion, finding that publication bias (in Asian countries) had skewed their results, and that acupuncture's efficacy in treating nausea did not exceed (but approximately equalled) that of antiemetic prophylaxis. Lee A, Copas JB, Henmi M, Gin T, Chung RC (2006). "Publication bias affected the estimate of postoperative nausea in an acupoint stimulation systematic review". J Clin Epidemiol. 59 (9): 980–3. doi:10.1016/j.jclinepi.2006.02.003. PMID 16895822.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Ezzo JM, Richardson MA, Vickers A; et al. (2006). "Acupuncture-point stimulation for chemotherapy-induced nausea or vomiting". Cochrane database of systematic reviews (Online) (2): CD002285. doi:10.1002/14651858.CD002285.pub2. PMID 16625560.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ Trinh K, Graham N, Gross A, Goldsmith C, Wang E, Cameron I, Kay T (2007). "Acupuncture for neck disorders". Spine. 32 (2): 236–43. doi:10.1097/01.brs.0000252100.61002.d4. PMID 17224820.
{{cite journal}}: CS1 maint: multiple names: authors list (link)Cochrane review of Acupuncture for neck disorders - ^ Acupuncture for idiopathic headache
- ^ Acupuncture for osteoarthritis
- ^ Mayhew E, Ernst E (2007). "Acupuncture for fibromyalgia--a systematic review of randomized clinical trials". Rheumatology (Oxford, England). 46 (5): 801–4. doi:10.1093/rheumatology/kel406. PMID 17189243.
- ^
McCarney, RW (2003). "Acupuncture for chronic asthma". Cochrane Database of Systematic Reviews. 2003 (3): CD000008. doi:10.1002/14651858.CD000008.pub2. Retrieved 2008-05-02.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^
He, L (2004). "Acupuncture for Bell's palsy". Cochrane Database of Systematic Reviews. 2007 (4): CD002914. doi:10.1002/14651858.CD002914.pub3. Retrieved 2008-05-02.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^
Gates, S (2006). "Auricular acupuncture for cocaine dependence". Cochrane Database of Systematic Reviews. 2006 (1): CD005192. doi:10.1002/14651858.CD005192.pub2. Retrieved 2008-05-02.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^
Smith, CA (2004-03-17). "Acupuncture for depression". Cochrane Database of Systematic Reviews. 2004 (3): CD004046. doi:10.1002/14651858.CD004046.pub2. Retrieved 2008-05-02.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^
Proctor, ML (2002). "Transcutaneous electrical nerve stimulation and acupuncture for primary dysmenorrhoea". Cochrane Database of Systematic Reviews. 2002 (1): CD002123. doi:10.1002/14651858.CD002123. Retrieved 2008-05-02.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^
Cheuk, DKL (2006). "Acupuncture for epilepsy". Cochrane Database of Systematic Reviews. 2006 (2): CD005062. doi:10.1002/14651858.CD005062.pub2. Retrieved 2008-05-02.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^
Law, SK (2007). "Acupuncture for glaucoma". Cochrane Database of Systematic Reviews. 2007 (4): CD006030. doi:10.1002/14651858.CD006030.pub2. Retrieved 2008-05-02.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Cheuk, DKL (2007). "Acupuncture for insomnia". Cochrane Database of Systematic Reviews. 2007 (3): CD005472. doi:10.1002/14651858.CD005472.pub2. Retrieved 2008-05-02.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Lim, B (2006). "Acupuncture for treatment of irritable bowel syndrome". Cochrane Database of Systematic Reviews. 2006 (4): CD005111. doi:10.1002/14651858.CD005111.pub2. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Smith, CA (2004). "Acupuncture for induction of labour". Cochrane Database of Systematic Reviews. 2004 (1): CD002962. doi:10.1002/14651858.CD002962.pub2. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Casimiro, L (2005). "Acupuncture and electroacupuncture for the treatment of rheumatoid arthritis". Cochrane Database of Systematic Reviews. 2005 (4): CD003788. doi:10.1002/14651858.CD003788.pub2. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Green, S (2005). "Acupuncture for shoulder pain". Cochrane Database of Systematic Reviews. 2005 (2): CD005319. doi:10.1002/14651858.CD005319. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Rathbone, J (2005). "Acupuncture for schizophrenia". Cochrane Database of Systematic Reviews. 2005 (4): CD005475. doi:10.1002/14651858.CD005475. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ White, AR (2006). "Acupuncture and related interventions for smoking cessation". Cochrane Database of Systematic Reviews. 2006 (1): CD000009. doi:10.1002/14651858.CD000009.pub2. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Zhang, SH (2005). "Acupuncture for acute stroke". Cochrane Database of Systematic Reviews. 2005 (2): CD003317. doi:10.1002/14651858.CD003317.pub2. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Wu, HM (2006). "Acupuncture for stroke rehabilitation". Cochrane Database of Systematic Reviews. 2006 (3): CD004131. doi:10.1002/14651858.CD004131.pub2. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Green, S (2002). "Acupuncture for lateral elbow pain". Cochrane Database of Systematic Reviews. 2002 (1): CD003527. doi:10.1002/14651858.CD003527. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Peng, WN (2008). "Acupuncture for vascular dementia". Cochrane Database of Systematic Reviews. 2007 (2): CD004987. doi:10.1002/14651858.CD004987.pub2. Retrieved 2008-05-06.
{{cite journal}}: Unknown parameter|coauthors=ignored (|author=suggested) (help) - ^ Tang JL, Zhan SY, Ernst E (1999). "Review of randomised controlled trials of traditional Chinese medicine". BMJ. 319 (7203): 160–1. PMID 10406751. Retrieved 2008-05-13.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Vickers A, Goyal N, Harland R, Rees R (1998). "Do certain countries produce only positive results? A systematic review of controlled trials". Control Clin Trials. 19 (2): 159–66. PMID 9551280.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ Lewith GT, White PJ, Pariente J (2005). "Investigating acupuncture using brain imaging techniques: the current state of play". Evidence-based complementary and alternative medicine : eCAM. 2 (3): 315–9. doi:10.1093/ecam/neh110. PMID 16136210. Retrieved 2007-03-06.
{{cite journal}}: Unknown parameter|month=ignored (help)CS1 maint: multiple names: authors list (link) - ^ "Report 12 of the Council on Scientific Affairs (A-97) -- Alternative Medicine". American Medical Association. 1997.
- ^ Haake M, Müller HH, Schade-Brittinger C; et al. (2007). "German Acupuncture Trials (GERAC) for Chronic Low Back Pain: Randomized, Multicenter, Blinded, Parallel-Group Trial With 3 Groups". Arch. Intern. Med. 167 (17): 1892–8. doi:10.1001/archinte.167.17.1892. PMID 17893311.
{{cite journal}}: Explicit use of et al. in:|author=(help)CS1 maint: multiple names: authors list (link) - ^ BBC NEWS, Acupuncture 'best for back pain'
- ^ Linde K, Streng A, Jürgens S, Hoppe A, Brinkhaus B, Witt C, Wagenpfeil S, Pfaffenrath V, Hammes MG, Weidenhammer W, Willich SN, Melchart D (2005). "Acupuncture for patients with migraine: a randomized controlled trial". JAMA. 293 (17): 2118–25. doi:10.1001/jama.293.17.2118. PMID 15870415.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Ann Intern Med - Rapid Responses for Scharf et al., 145 (1) 12-20
- ^ Lao L, Hamilton GR, Fu J, Berman BM (2003). "Is acupuncture safe? A systematic review of case reports". Alternative therapies in health and medicine. 9 (1): 72–83. PMID 12564354.
{{cite journal}}: CS1 maint: multiple names: authors list (link) - ^ Norheim AJ (1996). "Adverse effects of acupuncture: a study of the literature for the years 1981–1994". Journal of alternative and complementary medicine (New York, N.Y.). 2 (2): 291–7. PMID 9395661.
- ^ Leow TK (2001). "Pneumothorax Using Bladder 14". Medical Acupuncture. 16 (2).
- ^ Yekeler, Ensar. "Frequency of Sternal Variations and Anomalies Evaluated by MDCT". American Journal of Roentgenology. doi:10.2214. PMID 16554563. Retrieved 2007-11-24.
{{cite journal}}: Check|doi=value (help); Unknown parameter|coauthors=ignored (|author=suggested) (help); Unknown parameter|doi_brokendate=ignored (|doi-broken-date=suggested) (help) - ^ Be Wary of Acupuncture, Qigong, and "Chinese Medicine"
- ^ Final Report, Report into Traditional Chinese Medicine - NSW Parliament
- ^ Government of Ontario, Canada - News
- ^ http://www.e-laws.gov.on.ca/DBLaws/Statutes/English/06t27_e.htm
- ^ CTCMA
- ^ NCCAOM
- ^ "More than half of the physicians (59%) believed that acupuncture can be effective to some extent." Physicians Divided on Impact of CAM on U.S. Health Care; Aromatherapy Fares Poorly; Acupuncture Touted. HCD Research, 9 Sept. 2005. convenience link: Business Wire, 2005. Link to internet archive version: Cumulative Report
- ^ Updates-June 1996 FDA Consumer
- ^ US FDA/CDRH: Premarket Approvals
- ^ Traditional Chinese Medicine Act, 2006, S.O. 2006, c. 27
- ^ [1]]
- ^ Welcome to the Chinese Medicine Registration Board of Victoria
- ^ "Health NSW" (PDF).
External links