| |||
| |||
| Clinical data | |||
|---|---|---|---|
| Trade names | Adalat, Procardia, others | ||
| AHFS/Drugs.com | Monograph | ||
| MedlinePlus | a684028 | ||
| License data |
| ||
| Pregnancy category |
| ||
| Routes of administration | By mouth, topical | ||
| Drug class | Calcium channel blocker (dihydropyridine)[2] | ||
| ATC code | |||
| Legal status | |||
| Legal status | |||
| Pharmacokinetic data | |||
| Bioavailability | 45-56% | ||
| Protein binding | 92-98% | ||
| Metabolism | Gastrointestinal, Liver | ||
| Elimination half-life | 2 hours | ||
| Excretion | Kidneys: >50%, bile duct: 5-15% | ||
| Identifiers | |||
| |||
| CAS Number | |||
| PubChem CID | |||
| IUPHAR/BPS | |||
| DrugBank | |||
| ChemSpider | |||
| UNII | |||
| KEGG | |||
| ChEBI | |||
| ChEMBL | |||
| CompTox Dashboard (EPA) | |||
| ECHA InfoCard | 100.040.529 | ||
| Chemical and physical data | |||
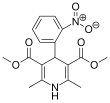
| Formula | C17H18N2O6 | ||
| Molar mass | 346.339 g·mol−1 | ||
| 3D model (JSmol) | |||
| Melting point | 173 °C (343 °F) | ||
| |||
| |||
| (verify) | |||
Nifedipine, sold under the brand name Procardia among others, is a calcium channel blocker medication used to manage angina, high blood pressure, Raynaud's phenomenon, and premature labor.[2] It is one of the treatments of choice for Prinzmetal angina.[2] It may be used to treat severe high blood pressure in pregnancy.[2] Its use in preterm labor may allow more time for steroids to improve the baby's lung function and provide time for transfer of the mother to a well qualified medical facility before delivery.[2] It is a calcium channel blocker of the dihydropyridine type.[2] Nifedipine is taken by mouth and comes in fast- and slow-release formulations.[2]
Common side effects include lightheadedness, headache, feeling tired, leg swelling, cough, and shortness of breath.[2] Serious side effects may include low blood pressure and heart failure.[2] Nifedipine is considered safe in pregnancy and breastfeeding.[5]
Nifedipine was patented in 1967, and approved for use in the United States in 1981.[2][6][7] It is on the World Health Organization's List of Essential Medicines.[8] It is available as a generic medication.[2] In 2021, it was the 128th most commonly prescribed medication in the United States, with more than 4 million prescriptions.[9][10]
Medical uses[edit]
High blood pressure[edit]
The approved uses are for the long-term treatment of hypertension and angina pectoris. In hypertension, recent clinical guidelines generally favour diuretics and ACE inhibitors, although calcium channel antagonists, along with thiazide diuretics, are still favoured as primary treatment for patients over 55 and black patients.[11]
Nifedipine given as sublingual administration has previously been used in hypertensive emergencies. It was once frequently prescribed on an as-needed basis to patients taking MAOIs for real or perceived hypertensive crises.[12] This was found to be dangerous, and has been abandoned. Sublingual administration of nifedipine promotes a hypotensive effect via peripheral vasodilation. It can cause an uncontrollable decrease in blood pressure, reflex tachycardia, and a steal phenomenon in certain vascular beds. There have been multiple reports in the medical literature of serious adverse effects with sublingual nifedipine, including cerebral ischemia/infarction, myocardial infarction, complete heart block, and death. As a result of this, in 1985 the FDA reviewed all data regarding the safety and effectiveness of sublingual nifedipine for the management of hypertensive emergencies, and concluded that the practice should be abandoned because it was neither safe nor effective.[13][14] An exception to the avoidance of this practice is in the use of nifedipine for the treatment of hypertension associated with autonomic dysreflexia in spinal cord injury.[15]
Early labor[edit]
Nifedipine has been used frequently as a tocolytic (agent that delays premature labor). A Cochrane review has concluded that it has benefits over placebo or no treatment for prolongation of pregnancy. It also has benefits over beta-agonists and may also have some benefits over atosiban and magnesium sulfate, although atosiban results in fewer maternal adverse effects. No difference was found in the rate of deaths among babies around the time of birth, while data on longer-term outcomes is lacking.[16]
Other[edit]
Raynaud's phenomenon is often treated with nifedipine. A 2005 meta-analysis showed modest benefits (33% decrease in attack severity, 2.8-5 reduction in absolute number of attacks per week); it does conclude that most included studies used low doses of nifedipine.[17]
Topical nifedipine has been shown to be as effective as topical nitrates for anal fissures.[18]
Nifedipine is also used in high-altitude medicine to treat high altitude pulmonary edema.[19]
Nifedipine is one of the main choices for the treatment of Prinzmetal angina due to its vasodilating effects on the coronary arteries.[2]
Other uses include painful spasms of the esophagus such as from cancer or tetanus.[medical citation needed] It is also used for the small subset of people with pulmonary hypertension.[medical citation needed]
Finally, nifedipine can be used in the treatment of renal calculi, which are commonly referred to as kidney stones. Studies have indicated that it helps to relieve renal colic. However, alpha blockers (such as tamsulosin) have been described as being significantly better.[20]
Side effects[edit]
Nifedipine rapidly lowers blood pressure, and patients are commonly warned they may feel dizzy or faint after taking the first few doses. Tachycardia (fast heart rate) may occur as a reaction. These problems are much less frequent in the sustained-release preparations of nifedipine.[medical citation needed]
Extended release formulations of nifedipine should be taken on an empty stomach, and patients are warned not to consume anything containing grapefruit or grapefruit juice, as they raise blood nifedipine levels. There are several possible mechanisms, including the inhibition of CYP3A4-mediated metabolism.[21]
As calcium channel blocker, nifedipine has a risk of causing gingival hyperplasia.[22]
Overdose[edit]
A number of persons have developed toxicity due to acute overdosage with nifedipine, either accidentally or intentionally, and via either oral or parenteral administration. The adverse effects include lethargy, bradycardia, marked hypotension and loss of consciousness. The drug may be quantified in blood or plasma to confirm a diagnosis of poisoning, or to assist in a medicolegal investigation following death. Analytical methods usually involve gas or liquid chromatography and specimen concentrations are usually in the 100-1000 μg/L range.[23][24]
Mechanism of action[edit]
Nifedipine is a calcium channel blocker. Although nifedipine and other dihydropyridines are commonly regarded as specific to the L-type calcium channel, they also possess nonspecific activity towards other voltage-dependent calcium channels.[25][26]
Nifedipine has additionally been found to act as an antagonist of the mineralocorticoid receptor, or as an antimineralocorticoid.[27]
History[edit]
Nifedipine (initially BAY a1040, then Adalat) was developed by the German pharmaceutical company Bayer, with most initial studies being performed in the early 1970s.[28]


Adalat was the first German pharmaceutical to be awarded the prestigious Prix Galien in 1980.[29] In the same year, Ahmed Hegazy submitted his invention (in collaboration with Klaus-Dieter Rämsch) of an extended release, solid medicinal preparation of nifedipine to the German Patent Office in Munich, patenting the "use of nifedipine crystals with a specific surface area of 1-4 m2/g for the production of solid medicinal formulations for achieving long-lasting blood levels for the oral treatment of hypertension by administration 1 to 2 times",[30] an invention that became known as Adalat retard from Bayer (see letter Dr Schauerte).[30] In that formulation, the active ingredient is released over a period of up to 36 hours.[31] With the increasing incidence of heart disease in that period—heart failure became the first cause of death in West Germany[32]—and the new formulation, the medication replaced Aspirin in the 1990s as the biggest single product of Bayer.[33] As Alexander Mey noted, "[d]iese Maßnahmen führten dazu, dass der Umsatz im Jahr 2000 auf 1,7 Mrd. US-$ stieg, obwohl das Präparat bereits ein Vierteljahrhundert am Markt war."[34] On 14 October 1991, Hegazy was awarded the Otto Bayer Medal—no relation to the company founder—for his work solubilizing poorly soluble active ingredients such as nifedipine, a prize, that the Bayer Group has been using to honor excellent research since 1984. By 2020, 528 researchers had received the award.[35] A 1995 US lawsuit, in which Hegazy defended his patent, found that Pfizer's Procardia XL product was also based on his European patent No. 0047899, United States Patent 5264446.[36]
The use of nifedipine and related calcium channel antagonists was much reduced in response to 1995 trials that mortality was increased in patients with coronary artery disease who took nifedipine.[37] This study was a meta-analysis, and demonstrated harm mainly in short-acting forms of nifedipine (that could cause large fluctuations in blood pressure) and at high doses of 80 mg a day and more.[38]
Society and culture[edit]
Brand names[edit]
In India, nifedipine is manufactured by JB Chemicals, and comes in brands Nicardia Retard (Nifedipine 10 mg, 20 mg tablets) and Nicardia XL 30/60, which are Nifedipine Extended Release tablets.[39]
In Switzerland, nifedipine is sold only as a generic version of extended release formulation, under the names Nifedipin Mepha and Nifedipin Spirig.[40]
References[edit]
- ^ "Nifedipine Pregnancy and Breastfeeding Warnings". Archived from the original on 21 December 2015. Retrieved 25 December 2015.
- ^ a b c d e f g h i j k l "Nifedipine". The American Society of Health-System Pharmacists. Archived from the original on 8 August 2018. Retrieved 17 September 2019.
- ^ "FDA-sourced list of all drugs with black box warnings (Use Download Full Results and View Query links.)". nctr-crs.fda.gov. FDA. Retrieved 22 October 2023.
- ^ "Product monograph brand safety updates". Health Canada. February 2024. Retrieved 24 March 2024.
- ^ "Nifedipine". Drugs and Lactation Database. Bethesda (MD): National Institute of Child Health and Human Development. 15 August 2023. PMID 30000106. Retrieved 14 October 2023.
- ^ Sliskovic DR (2013). "Cardiovascular Drugs". In Li JJ, Corey EJ (eds.). Drug Discovery: Practices, Processes, and Perspectives. Hoboken, NJ: John Wiley & Sons. pp. 141–204. ISBN 9781118354469. Archived from the original on 1 September 2017. Retrieved 20 January 2022. p. 172:
nifedipine...1,4-dihydropyrine originally approved in 1981.
- ^ Fischer J, Ganellin CR (2006). Analogue-based Drug Discovery. John Wiley & Sons. p. 464. ISBN 9783527607495.
- ^ World Health Organization (2019). World Health Organization model list of essential medicines: 21st list 2019. Geneva: World Health Organization. hdl:10665/325771. WHO/MVP/EMP/IAU/2019.06. License: CC BY-NC-SA 3.0 IGO.
- ^ "The Top 300 of 2021". ClinCalc. Archived from the original on 15 January 2024. Retrieved 14 January 2024.
- ^ "Nifedipine - Drug Usage Statistics". ClinCalc. Retrieved 14 January 2024.
- ^ Hypertension: management of hypertension in adults in primary care. Clinical guideline CG34. National Institute for Health and Clinical Excellence (NICE). June 2006. ISBN 1-86016-285-1. Archived from the original on 17 June 2007.
- ^ Gelenberg AJ (March 1997). "Nifedipine for MAOI Hypertension? Reversing a Previous Recommendation". Biological Therapies in Psychiatry. Archived from the original on 10 September 2015. Retrieved 22 January 2015 – via Dr. Bob's Psychopharmacology Tips.
- ^ Grossman E, Messerli FH, Grodzicki T, Kowey P (1996). "Should a moratorium be placed on sublingual nifedipine capsules given for hypertensive emergencies and pseudoemergencies?". JAMA. 276 (16): 1328–1331. doi:10.1001/jama.1996.03540160050032. PMID 8861992.
- ^ Varon J, Marik PE (October 2003). "Clinical review: the management of hypertensive crises". Critical Care. 7 (5): 374–384. doi:10.1186/cc2351. PMC 270718. PMID 12974970.
- ^ Campagnolo DI. "Autonomic Dysreflexia in Spinal Cord Injury". eMedicine. Retrieved 14 July 2011.
- ^ Flenady V, Wojcieszek AM, Papatsonis DN, Stock OM, Murray L, Jardine LA, et al. (June 2014). "Calcium channel blockers for inhibiting preterm labour and birth". The Cochrane Database of Systematic Reviews. 2014 (6): CD002255. doi:10.1002/14651858.CD002255.pub2. PMC 7144737. PMID 24901312.
- ^ Thompson AE, Pope JE (February 2005). "Calcium channel blockers for primary Raynaud's phenomenon: a meta-analysis". Rheumatology. 44 (2): 145–150. doi:10.1093/rheumatology/keh390. PMID 15546967.
- ^ Ezri T, Susmallian S (June 2003). "Topical nifedipine vs. topical glyceryl trinitrate for treatment of chronic anal fissure". Diseases of the Colon and Rectum. 46 (6): 805–808. doi:10.1007/s10350-004-6660-8. PMID 12794583. S2CID 24717470.
- ^ Ali MO, Qazi S (19 September 2007). "Pulmonary Edema, High-Altitude". eMedicine. Archived from the original on 16 November 2007. Retrieved 25 November 2007.
- ^ Bos D, Kapoor A (November 2014). "Update on medical expulsive therapy for distal ureteral stones: Beyond alpha-blockers". Canadian Urological Association Journal = Journal de l'Association des Urologues du Canada. 8 (11–12): 442–445. doi:10.5489/cuaj.2472. PMC 4277526. PMID 25553160.
- ^ Odou P, Ferrari N, Barthélémy C, Brique S, Lhermitte M, Vincent A, et al. (April 2005). "Grapefruit juice-nifedipine interaction: possible involvement of several mechanisms". Journal of Clinical Pharmacy and Therapeutics. 30 (2): 153–158. doi:10.1111/j.1365-2710.2004.00618.x. PMID 15811168. S2CID 30463290.
- ^ "Nifedipine". NICE. Retrieved 1 April 2021.
- ^ Nifediac package insert, TEVA Pharmaceuticals, Sellersville, Pennsylvania, August 2009.
- ^ Baselt RC (2008). Disposition of Toxic Drugs and Chemicals in Man. Foster City, CA: Biomedical Publications. pp. 1108–1110. ISBN 978-0-9626523-7-0.
- ^ Curtis TM, Scholfield CN (May 2001). "Nifedipine blocks Ca2+ store refilling through a pathway not involving L-type Ca2+ channels in rabbit arteriolar smooth muscle". The Journal of Physiology. 532 (Pt 3): 609–623. doi:10.1111/j.1469-7793.2001.0609e.x. PMC 2278590. PMID 11313433.
- ^ McDonald TF, Pelzer S, Trautwein W, Pelzer DJ (April 1994). "Regulation and modulation of calcium channels in cardiac, skeletal, and smooth muscle cells". Physiological Reviews. 74 (2): 365–507. doi:10.1152/physrev.1994.74.2.365. PMID 8171118.
- ^ Luther JM (September 2014). "Is there a new dawn for selective mineralocorticoid receptor antagonism?". Current Opinion in Nephrology and Hypertension. 23 (5): 456–461. doi:10.1097/MNH.0000000000000051. PMC 4248353. PMID 24992570.
- ^ Vater W, Kroneberg G, Hoffmeister F, Saller H, Meng K, Oberdorf A, et al. (January 1972). "[Pharmacology of 4-(2'-nitrophenyl)-2,6-dimethyl-1,4-dihydropyridine-3,5-dicarboxylic acid dimethyl ester (Nifedipine, BAY a 1040)]". Arzneimittel-Forschung (in German). 22 (1): 1–14. PMID 4622472.
- ^ Lichtlen PR (1991). Adalat: A Comprehensive Review. Berlin et al: Springer-Verlag. p. 2. ISBN 3642855008.
- ^ a b EP 0047899B2, Hegasy A, Rämsch KD, "Solid pharmaceutical compositions containing nifedipine, and process for their preparation", issued 28 February 1996, assigned to Bayer AG
- ^ "Adalat Retard Tablet". tabletwise.net. Retrieved 29 January 2022.
- ^ "Herzversagen Todesursache - Sterbefälle Sterbeziffern 1980-1997". www.gbe-bund.de. Retrieved 29 January 2022.
- ^ Bletzer S (2 July 2013). Pharma-Unternehmen und Gesundheitsmanagement: Strategische Diversifizierung durch Dienstleistungen (in German). Springer-Verlag. pp. 8, footnote 49. ISBN 978-3-322-99515-5.
- ^ Mey A (2013). Drees N (ed.). "Pharmamarketing: Rx-to-OTC-Switch als strategischer Ansatz im Life-Cycle-Management für pharmazeutische Produkte" (PDF). Erfurter Hefte zum Angewandten Marketing (in German) (40). Erfurt, Deutschland: Fachhochschule Erfurt University of Applied Sciences Wirtschafts-wissenschaften: 1–56, esp. 17. Retrieved 8 March 2021 – via DB-Thueringen.de.
- ^ "The Otto Bayer Medal". Science Prize for Bayer Employees. 3 January 2022. Retrieved 29 January 2022.
- ^ "Pfizer Found Guilty In Adalat CC Case". The Pharma Letter. London. 4 September 1994. Retrieved 29 January 2022.
- ^ Furberg CD, Psaty BM, Meyer JV (September 1995). "Nifedipine. Dose-related increase in mortality in patients with coronary heart disease". Circulation. 92 (5): 1326–1331. doi:10.1161/01.cir.92.5.1326. PMID 7648682. S2CID 32044931.
- ^ Opie LH, Messerli FH (September 1995). "Nifedipine and mortality. Grave defects in the dossier". Circulation. 92 (5): 1068–1073. doi:10.1161/01.cir.92.5.1068. PMID 7648646.
- ^ "Nicardia XL". Medical Dialogues. Retrieved 24 February 2021.
- ^ "Compendium". Retrieved 10 February 2023.